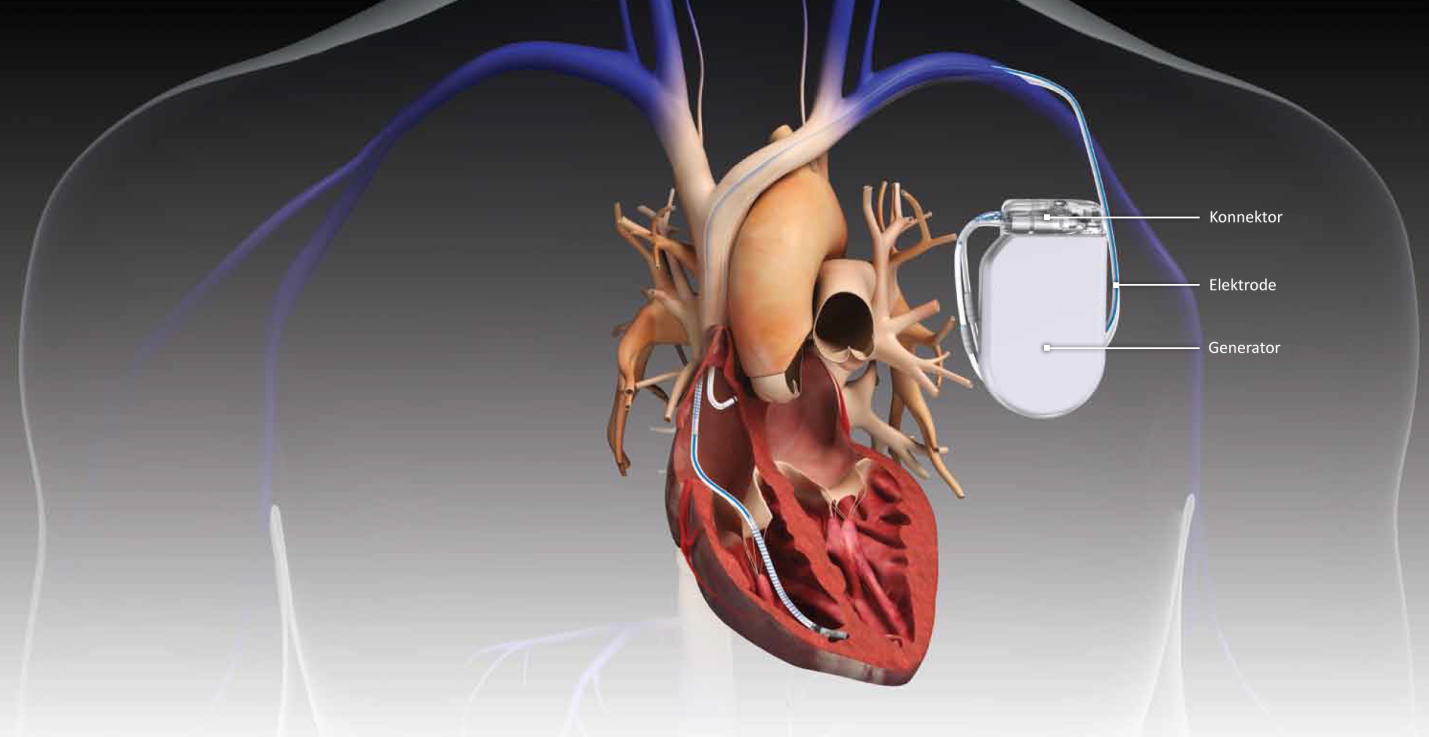
Medical implants for cardiac arrhythmia:
Various diseases or changes in the heart can cause a disturbance of the heart rhythm. Examples of arrhythmia are an extremely slow heart rate, skipping beats, or exceptionally fast beats per minute. The most commonly used implants in the treatment of cardiac arrhythmias are the pacemaker and the ICD.
The Pacemaker
People who suffer from heart arrhythmias that cause slow heartbeats use a pacemaker. The pacemaker is inserted subcutaneously in the front of the shoulder, under the clavicle, and connected to the heart with electrodes (leads). A pacemaker may consist of one to three wires, which, in the case of multiple cables, are each connected to a different ventricle [46]. The pacemaker continuously supports the heart rate. When an anomaly in the heart rhythm occurs, the pacemaker delivers an electrical stimulus from within the pulse generator that will restore the normal heart rhythm [36]. This correction is done automatically with the aid of a sensor, an electronic circuit that looks like a small computer, which monitors the cardiac rhythm [45]. A battery powers the pacemaker and can last on average between six and ten years [40].
For better functionality, pacemakers today have a radio station built-in that makes it possible for physicians and patients to wirelessly adjust the settings outside the body, but also to check the operations of the pacemaker itself. People who have a pacemaker will require periodic clinical check-ups to provide information regarding, the functioning of the pacemaker leads, the frequency of utilization of the pacemaker, and the battery life to check whether the pacemaker is functioning properly. Within these check-ups, an antenna (programmer) is placed on top of the chest to make contact with the chip inside the pacemaker. The data can be read using an ECG device that provides an overview of the functioning of the heart. An additional advantage of this virtual accessibility is that doctors can collect data on a large scale to improve medical care.
Implantable Cardioverter-defibrillator
An Implantable cardioverter-defibrillator (ICD) is used by patients who suffer from more dangerous, unpredictable arrhythmia and are at risk of sudden cardiac arrest. Although an ICD has a built-in pacemaker and is also placed under the skin on the front of the shoulder under the clavicle, it’s more sophisticated and slightly larger than a standard pacemaker. With the built-in pacemaker, it can come into action when a slow heartbeat occurs, but because of the more sophisticated features, it’s also able to intervene in situations where the heart rhythm is too fast or by a cardiac arrest [42]. The ICD attempts to restore the rhythm of the heart if the arrhythmia is not life-threatening. When the heart does not respond to this, the ICD gives a shock which is repeated every 10 to 15 seconds to restore the rhythm, in most cases two shocks are sufficient [40:1].
Patients with an ICD need periodic clinical check-ups as well to check the performance of the battery and to read out the memory on the chip. The average Dutch patient goes twice a year to the hospital for clinical check-ups. Nowadays, it is also possible to perform a clinical check-up remotely, also referred to as home-monitoring or telemonitoring [40:2]. The patient receives a monitoring system to take home and connects it to a fixed line or mobile network. This new development makes earlier intervention possible in case the ICD isn’t functioning properly. It can be programmed to check its features every night without the patient noticing anything, to ensure the additional technical safety of the ICD [41]. This test checks whether the battery is still full enough, how the wires work if the heart rhythm is normal, and whether the medication is working properly. These data are stored in the memory of the ICD, forwarded to a secure server, and saved in a database [40:3]. It gives a beeping sound if it finds an error during a check-up [55]. In such cases, the cardiologist or technician receives a message through text or e-mail.